Book Appointment Now

The Story of Inflammation…
Lately, we seem to hear the word inflammation more and more often.
Reducing inflammation. Increasing inflammation.
We recognise the warm limb, the pain, the burning sensation, the fatigue, the mental fog… but how do we get there? And most importantly, get out?
What is actually happening inside the body?..
What is inflammation? …
In a galaxy far, far away…
Which is not so far away at all, because it exists directly within you…
Billions of processes unfold when your doctor says: “inflammation.”
Inflammation is the body’s protective response to a threat, injury, or the presence of a foreign substance.
Its purpose is to:
- eliminate the danger
- repair the damaged area
- restore balance
Triggers of inflammation
Foreign invaders (external origin):
- bacteria
- viruses
- fungi
- toxins
Tissue damage (internal origin):
Examples include:
- oxidative stress (an excess of free radicals — molecules with unpaired electrons)
- mechanical injury
- toxic metabolic by-products*
- excessive intake of fat, sugar, or alcohol
Misplaced molecules
Substances that are normally contained but appear in the wrong location.
Examples:
- bacterial fragments leaking from the gut (e.g. LPS)
- debris from dead cells
- crystals (such as uric acid)
When such signals occur in the course of everyday life, how do they translate into inflammation?
The cell signals: “I am injured.”
On the surface and within the interior of cells, there are specialised sensors.
What are these sensors?
They are molecular structures located on the cell membrane (or inside the cell) that bind specific signalling molecules — such as hormones or neurotransmitters. Through these interactions, the cell receives information about changes in its environment and initiates appropriate responses, including cell division, metabolic adjustments, or the transmission of signals within the nervous system.
How do these mechanisms work?
A signalling molecule binds specifically to its surface receptor.
This binding alters the receptor’s structure.
That structural shift initiates an intracellular signalling cascade, which ultimately reaches the nucleus and induces change.
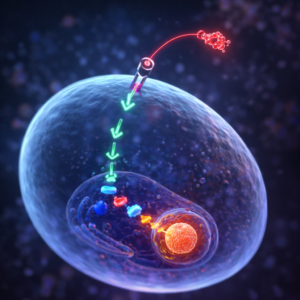
There are countless signalling pathways,
but the ones we need to focus on here have weird names like:
NF-κB (nuclear factor kappa B)
MAPK pathways (mitogen-activated protein kinases)
NF-κB is present in nearly all animal cells and plays a pivotal role in regulating DNA transcription, particularly in immune responses, inflammation, cell growth, stress reactions, and cell survival. It is activated by stimuli such as cellular stress, infections (bacterial or viral), and cytokines. Upon activation, NF-κB translocates to the nucleus, where it modulates the expression of hundreds of genes involved in processes ranging from host defence to tumour biology.
Imagine DNA sitting quietly and contentedly within the cell.
Then along comes a “transcription factor, announcing: “there is danger”.
Inflammatory proteins and enzymes must be produced to confront it.
Within the DNA, transcription and translation are initiated — processes deserving of their own dedicated discussion.
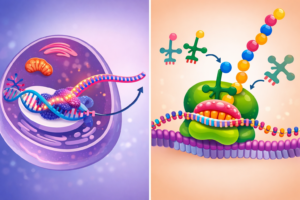
The key point is this:
the segments of genes required to address the threat are selectively copied.
As a result, enzymes and proteins are synthesised that enable the cell to mount its defensive response.
An important nuance:
Almost every cell in the body contains the same genome, yet not all genes are active simultaneously.
During inflammation, the transcription of specific genes is amplified. A cell expresses only those genes necessary for its immediate needs.
Thus, the cell begins to:
– produce cytokines
– synthesise COX-2 and iNOS
– create a pro-inflammatory environment
What are cytokines?
Cytokines are small but crucial signalling proteins — the messengers and coordinators of the immune response.
Their primary functions include:
– orchestrating communication between immune cells
– recruiting immune cells to sites of infection or injury
– initiating and sustaining inflammation
– later contributing to the resolution of inflammation and tissue repair
Immune cells, such as lymphocytes and macrophages, “speak” to one another through cytokines, alerting the system when an invader has been detected.

How do cytokines exert their effects?
For example:
– They dilate blood vessels and increase vascular permeability. This allows plasma and immune cells to enter tissues, producing the characteristic redness and swelling.
– They attract white blood cells (such as neutrophils and macrophages) to the precise location where action is required.
– Certain cytokines act on the brain’s thermoregulatory centre, inducing fever. Elevated body temperature enhances immune efficiency and can inhibit pathogen replication.
COX-2 and iNOS — what are they?
They are enzymes responsible for generating inflammatory mediators:
COX-2 → produces prostaglandins
iNOS → produces nitric oxide (NO)
What do these mediators do?
– Vasodilation
Prostaglandins relax vascular smooth muscle, widening blood vessels → increased blood flow.
– Pain sensitisation
Nitric oxide enhances the sensitivity of pain receptors → even minor stimuli become painful.
Picture communication between nerve cells as a calm conversation between two rooms. Under normal conditions, the message (pain) passes through at a moderate volume.
In inflammation, nitric oxide turns the conversation into shouting.
The same signal now sounds far louder.
Neurons effectively “raise their voices,” amplifying pain perception.
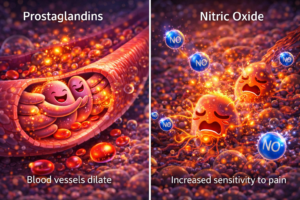
Inflammation becomes visible and tangible in the skin because mediators dilate vessels, bring warm blood to the surface, allow fluid to escape into tissues, and sensitise nerve endings. The result: warmth, redness, swelling, and pain.
In internal organs, inflammation may be felt instead as:
– tension
– pressure
– discomfort
For instance, in the gut:
smooth muscle spasms, gas formation, and pain — all consequences of these microscopic mediators.
When inflammation subsides…
We can imagine the same system at work, but with different molecular actors.
A signal binds to a receptor →
the protein cascade delivers a new message to the DNA →
different gene segments are transcribed →
“repair crews” are produced.

The anti-inflammatory programme is activated.
The body generates counter-signals, including:
IL-10 (Interleukin-10)
Often described as a master regulator, IL-10 directly suppresses pro-inflammatory immune cells, signalling that the active phase of defence should cease.
TGF-β (Transforming Growth Factor beta)
Dampens immune activity while stimulating collagen synthesis and tissue repair.
Lipoxins and resolvins
Derived from omega-3 fatty acids, these molecules actively promote resolution by clearing excess immune cells and inflammatory debris.
Late-phase Prostaglandin E₂
A fascinating paradox: the same molecule that initially contributes to pain and vasodilation later helps reprogramme cells towards healing.
Collectively, these mediators:
– inhibit inflammatory gene expression
– reduce immune cell activation
– promote regeneration and recovery
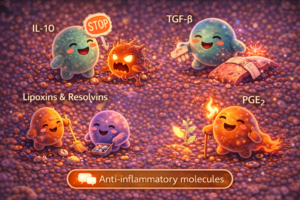
Notably, they utilise many of the same signalling routes as pro-inflammatory mediators — yet press different molecular “buttons” within the nucleus.
Here, another pathway becomes central: STAT3 (Signal Transducer and Activator of Transcription 3)
Some basic Nutritional connections
Selenium — the pathway’s “cleaner”
For anti-inflammatory signals to efficiently reach the nucleus, intracellular conditions must remain balanced.
Excess free radicals can disrupt signalling pathways, delaying or distorting messages. (free radicals are molecules, which miss an electron, so they’ve decided to go around and steal it from all the other well-working molecules. This way free radicals harm them, and the rest of the molecules can’t function properly anymore… so an important thing is to stop them!
Selenium is an essential component of glutathione peroxidase, a key antioxidant enzyme that neutralises reactive species such as hydrogen peroxide (H₂O₂ → H₂O).
Adequate selenium supports redox balance and preserves signalling fidelity.
A potent dietary source remains Brazil nuts — typically 1–2 per day is sufficient.
Vitamin C: The Courier’s “Refreshment”
Protecting the DNA
When an anti-inflammatory “courier” signal – for instance via IL-10 – enters the nucleus, the DNA must briefly adopt an open configuration so that healing and repair genes can be read. In this exposed state, however, DNA becomes highly vulnerable. Vitamin C stands guard within the nucleus, helping to shield genetic material from the “splash damage” caused by invading free radicals.
Reinforcing the command
Vitamin C also assists the function of specific enzymes known as demethylases. These enzymes remove inhibitory chemical marks from DNA – molecular “brakes” that might otherwise hinder cellular repair and resolution of inflammation.
And if that were not enough…
Neutralising free radicals
Free radicals are unstable molecules that “steal” electrons from surrounding structures, thereby damaging cells. Vitamin C can donate its own electrons, stabilising these reactive species and preventing further harm. This electron-donating capacity is a defining feature of antioxidants as a group.



We can think about a practical question… How Does Vitamin C Enter the Cell?
How does Vitamin C from lemon juice or a multivitamin actually gain entry into a cell?
Cell membranes are equipped with transport systems – microscopic pumps and gateways that import essential molecules. One of particular interest here is GLUT1, primarily responsible for transporting glucose into the cell.
During inflammation, oxidised Vitamin C adopts a form called dehydroascorbic acid (DHA). In this state, it closely resembles glucose in structure. GLUT1, unable to fully distinguish between them, transports DHA across the membrane. Once inside the cell, DHA is converted back into active Vitamin C, ready to perform its protective functions.
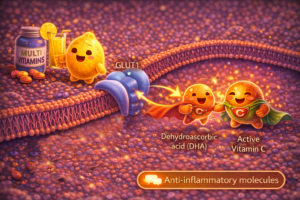
Vitamin C can “masquerade” as sugar because both molecules share a similar six-carbon backbone. In the metabolic intensity of inflammation, cells increase glucose transport – and in doing so, they inadvertently import the protective vitamin through the same gateway.
What appears to be a case of mistaken identity ultimately serves a beneficial purpose: enabling Vitamin C to reach precisely those cells that need antioxidant defence the most.
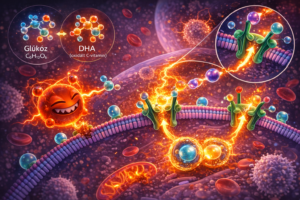
That is why sugar intake matters during illnesses
This mechanism carries an important implication.
When you eat a large amount of sweets sugar, cakes, pastries, sugary drinks … glucose and Vitamin C must compete for the same transport pathways. Excess sugar effectively crowds out Vitamin C, reducing its cellular uptake.
During periods of infection or active inflammation, limiting refined sugar intake becomes particularly important.
Without this adjustment, even adequate Vitamin C consumption may not translate into effective delivery to immune cells.
The next part of this story is about how particular foods can contribute to lower the level of inflammation on a cellular level.
Later on we talk about the opposite, what kind of eating habits lead to disharmony and inflammation.
But if you are only interested in the practical part, click here for the most important foods, considering inflammation.
Sources
- pubmed.ncbi.nlm.nih.gov (NF-κB signaling in inflammation)
- www.ncbi.nlm.nih.gov (Curcumin and NF-κB inhibition)
- pubmed.ncbi.nlm.nih.gov (Cytokines: the language of the immune system)
- www.nature.com (Cytokine-storm: mechanisms and treatments)
- pubmed.ncbi.nlm.nih.gov (The role of IL-6 in chronic inflammation)
- www.sciencedirect.com
- pubmed.ncbi.nlm.nih.gov (Nitric oxide and NMDA receptor in pain)
- www.sciencedirect.com
- pubmed.ncbi.nlm.nih.gov (NO and pro-inflammatory signaling)
- pubmed.ncbi.nlm.nih.gov (Zinc and immune function)
- pubmed.ncbi.nlm.nih.gov (Selenium and Glutathione Peroxidase activity)
- www.ncbi.nlm.nih.gov (Magnesium and inflammation)
- pubmed.ncbi.nlm.nih.gov (Vitamin C and GLUT1 transport in immune cells)
